Each year about 780,000 people experience a new or recurrent stroke. Nearly a third never regain their ability to walk independently again (American Heart Association--Heart Disease and Stroke Statistics, Update 2008).
One of the leading causes of difficulty walking after a stroke is foot drop, a weakness or paralysis of the muscles that lift the front of the foot. People with foot drop often drag their foot and hike their hip to take a step, causing long-term damage and making walking miserable.
Ocean Springs Hospital Neurological Rehabilitation has helped numerous patients recover from stroke and neurological damage. Despite access to a century's worth of rehabilitative therapies, the staff had not found a device that met the full spectrum of rehabilitative needs for treatment of foot drop, such as impaired dorsiflexion, stance-limb stability and muscle stimulation to avoid atrophy.
However, a recent advance in the field of neurostimulation is offering hope to many stroke patients with foot drop. In July 2008, Ocean Springs Hospital Neurological Rehabilitation integrated into its rehabilitation programs the next generation in functional electrical stimulation (FES), which uses low levels of electrical current to stimulate nerves and innervate the extremities.
FES is not a cure for stroke damage, but by directly stimulating nerve fibers, it addresses musculoskeletal limitations and corrects foot drop.
In the past, the only effective technology that treated foot drop was a hard plastic ankle-foot orthosis (AFO) worn around the leg to manage any dysfunction of the ankle or foot during ambulation. AFOs, however, may cause other problems, including ankle joint stiffness, skin breakdown around the orthosis, muscle atrophy in the ankle region, and degenerative joint problems in the hip due to a compensatory motion known as "hip hike."
Moreover, patients using AFOs often find them uncomfortable to wear, resulting in poor user compliance.
Thankfully, science has developed FES, which uses electrical impulses to activate specific muscles and mimic "normal patterning" to allow patients to lift their foot and clear a step.
FES At Work:
The NESS L300™
The NESS L300 is a leading FES device that directly stimulates nerve fibers to address musculoskeletal limitations and correct foot drop. Candidates include patients with stroke, traumatic brain injury, incomplete spinal cord injuries, and other disorders of the central nervous system that result in functional deficits and impairments of the lower limb.
The FDA-approved NESS L300 has three main parts that use wireless communication to "talk" to each other.
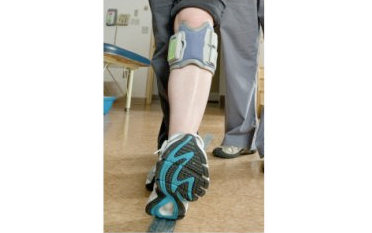
Comfortable, Lightweight Functional Stimulation Cuff: The leg cuff is a small, light-weight device that fits just below the knee and contains electrodes designed to place stimulation where it helps the patient most.
Innovative Intelli Sense Gait Sensor™: The gait sensor attaches to the shoe and lets the leg cuff know if the heel is on the ground or in the air. The gait sensor can be transferred to different shoes easily; a quality that patients truly appreciate, especially after dealing with cumbersome AFOs.
Wireless, Portable Control Unit: The hand-held remote control lets patients and their physical therapists adjust the level of stimulation and turn the unit on and off.
When a patient tries to walk, the NESS L300 sends electronic signals to stimulate the peroneal nerve which, in turn, signals under-active muscles to help patients lift their foot off the ground and walk more normally.
Most patients who have purchased the NESS L300 for home therapy use it regularly. A key feature of the NESS L300 is a built-in training mode that is designed to improve conditioning and control of the ankle dorsiflexors.
This conditioning program completed daily has been shown to improve the controlled strength in most patients and improve gait velocity and improved symmetry of stance.
One Case in Point
When Mrs. S., 65, arrived at our multidisciplinary clinic, she was wheelchair-bound following a hemorrhagic MCA CVA with resulting right hemiparesis that occurred two months earlier.
She had already participated in extensive inpatient rehabilitation and demonstrated significant sensory and perceptual deficits, severe right lower-extremity edema and hip pain, lack of force production, and poor voluntary movement in the right lower extremity in supine at less than 50 percent that of the left side.
She also required assistance for upright sitting without trunk support, moderate assistance for bed mobility and transfers, and maximal assistance to stand in the parallel bars with severely flexed posture and minimal to no weight bearing through the right lower extremity.
My initial therapy prognosis was good for return to gait at household distances with minimal assistance in six months. Luckily for Mrs. S. and all the patients to enter our clinic after her, Ocean Springs had purchased the Bioness NESS L300 that summer.
The Bioness clinical specialist in our region suggested we try the unit on Mrs. S., but I was skeptical. Initially we only used the unit to work on sensory feedback for stance. But in two short sessions the NESS L300 helped Mrs. S. support herself better in stance. Her early gait training required an unweighing harness, the NESS L300 and two therapists on the ground.
Mrs. S. regained full voluntary movement in her right ankle but we continued to use the NESS L300 for sensory information and to reduce incoordination, especially during activities that allowed her less cognitive attention to her right side.
At her discharge in six months, Mrs. S. was ambulating community distances at a speed of .3 m/sec with a straight cane with CGA or at .5 m/sec and supervision with a rolling walker. Her Berg Balance Score was a 45/56; at initial evaluation this was not even an appropriate test for her. The assistance she required was due to impaired decision making skills and residual right neglect.
Mrs. S. never truly understood what the NESS L300 did for her, but from a therapist's perspective, I knew that her excellent mobility outcomes were largely due to this innovative device. At a six-month follow-up assessment, Mrs. S. had further increased her gait speed with a cane to .5 /sec.
Every day we see new patients aided by the NESS L300. Often they are patients who we have seen in the past and are interested in trying this new technology either in the clinic or at home.
Application for Physical Therapists
Though the obvious application of the NESS L300 is for dorsiflexion during gait, the benefits of this tool stretch far beyond just walking. Drop foot is hardly ever the only deficit leading to gait difficulty and often when the NESS L300 is doing its job, it becomes even more apparent where the patient is in need of PT skills for facilitation at the trunk or hip. It allows the therapist to attend to multiple areas and problem-solve, and treat the gait abnormality.
The NESS L300 can be set in gait mode, where the peroneal nerve is stimulated when the heel is non-weight bearing; training mode, where custom set on/off times are in place; or in clinician mode, where stimulation is supplied when the therapist/patient desires for as long as the remote control is depressed.
Using either the training or clinician mode, the therapist can further promote voluntary movement in a paretic limb. For example, during a heel slide, a patient who cannot initiate the movement without FES can often not only initiate but also complete most of the movement with the NESS L300. This reduces undesired compensatory movements and allows the patient to relearn the proper movement. Traditional electrical stimulation devices, though useful, are typically not as user-friendly.
The NESS L300 is also invaluable when relearning smooth, controlled movement from sitting to standing, as it helps initiate the proper forward momentum and muscle recruitment pattern with anterior tibialis activation. It also encourages proper weight shift and weight bearing through increased sensory feedback.
The device can also be used to help cue for bed mobility during elevating the lower extremities to the bed, moving them over, or even during bridging to adjust oneself. Many patients comment on the increased ease of all of these movements with the help of the NESS L300. In addition, patients using the NESS L300 to replace their AFOs also comment on the energy cost savings; they can typically ambulate further and longer with less fatigue.
I believe we have always offered exceptional care in our clinic at Ocean Springs. The NESS L300 has allowed us to help provide a greater return to functional mobility and independence to even more patients.
Ashley Campbell is a physical therapist at Ocean Springs Hospital Neurological Rehabilitation, Ocean Springs, MS.